You are eating whole foods, going to the gym, trying intermittent fasting, and doing everything “right”, yet the number on the scale refuses to budge. Worse still, you might feel exhausted, constantly hungry, and increasingly frustrated with your body. This is unfortunately a common scenario we see with our clients who have been diagnosed with Polycystic Ovary Syndrome (PCOS).
Recently, the conversation around Ozempic and PCOS weight loss has shifted towards weight loss injections, with GLP-1 medications like Ozempic and Wegovy often positioned as a breakthrough solution.
But what are these drugs actually doing, and can those same effects be achieved naturally for PCOS?
Why Weight Gain Is So Common in PCOS
If you find it difficult to lose weight with PCOS, you may feel relieved to know that it’s not a willpower problem: your hormones are likely playing a role. For women with PCOS, weight gain is strongly linked to the following mechanisms:
Insulin resistance and fat storage
Research suggests that up to 70 percent of women with PCOS have insulin resistance, which plays a central role in weight gain and difficulty losing weight. According to the NHS, insulin resistance is one of the key drivers of PCOS symptoms, including weight changes.
Insulin is the hormone that allows your cells to absorb glucose for energy. In insulin resistance, your cells stop responding effectively, so your body produces more insulin to compensate. High insulin levels block fat burning and promote fat storage, particularly around the abdomen. Learn more about insulin resistance.
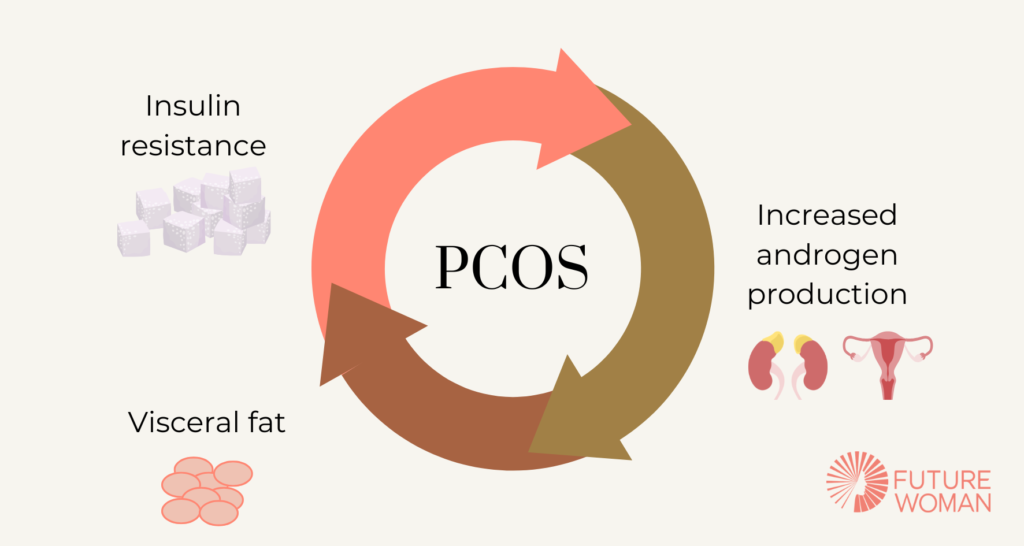
Elevated insulin increases androgens
High insulin levels also stimulate the ovaries to produce more androgens such as testosterone. This further drives fat accumulation, especially visceral fat, and contributes to the hormonal imbalance seen in PCOS.
Blood sugar instability and cravings
When blood sugar fluctuates, it creates energy crashes and strong cravings for sugar and refined carbohydrates, making weight loss even harder.
The role of stress and cortisol
Chronic stress, often present in women with PCOS, increases cortisol, which raises blood sugar, worsens insulin resistance, and encourages fat storage around the midsection. Read more about the role of stress on hormone health.
What GLP-1 Medications Actually Do
To understand the rise of Ozempic for PCOS, it helps to look at how GLP-1 medications work.
These drugs mimic a natural hormone called GLP-1 and influence several key systems in the body:
- They slow gastric emptying, meaning food stays in your stomach for longer
- They reduce appetite signals, helping you feel fuller with less food
- They improve insulin response, supporting better blood sugar control
- They stabilise blood sugar levels, reducing spikes and crashes
In simple terms, they reduce hunger and improve metabolic function at the same time.
Why Ozempic Works for PCOS Weight Loss
This is why Ozempic PCOS weight loss has become such a widely discussed topic: GLP-1 medications may be effective because they directly target the underlying metabolic dysfunction in PCOS.
By improving insulin sensitivity and stabilising blood sugar, they create a more favourable hormonal environment. Appetite is reduced, which makes it easier to maintain a calorie deficit without relying on willpower.
Research also shows that GLP-1 medications can reduce androgen levels and support more regular ovulation.
The Limitations of GLP-1 Medications
While these medications can be helpful, their benefits are largely limited to the period of use. Once stopped, the effects on appetite, blood sugar, and weight typically reverse, and there is currently limited long-term safety data for sustained use.

They do not address the underlying root cause
GLP-1s manage appetite and blood sugar, but they do not resolve the underlying drivers of PCOS such as inflammation, gut health, or chronic stress.
Weight rebounding is common
After stopping Ozempic and other GLP-1 medications, research shows that weight regain is rapid in the first 6–12 months and then slows over time, with around half to two-thirds of lost weight regained overall. In some studies, this level of regain occurred even with ongoing lifestyle counselling, highlighting that the underlying drivers of weight gain often remain unaddressed.
Risk of muscle loss
Rapid weight loss can lead to loss of muscle mass, which is particularly problematic as muscle plays a key role in insulin sensitivity and metabolism.
Digestive side effects
Nausea, bloating, and digestive discomfort are common, particularly in the early stages.
Risk of nutrient deficiencies
Studies show GLP-1s predispose users to micronutrient deficiencies through appetite suppression, delayed gastric emptying and altered absorption, with vitamin D, iron and calcium most at risk.
Increase in pregnancy risk factors
Emerging research has shown an increase in pregnancy risk factors in mothers who took GLP-1s prior to pregnancy including a higher rate of gestational diabetes, preterm birth, hypertensive disorder and excess weight gain during pregnancy.
No medium term to long term safety data
Finally, a recent narrative review noted that there is still limited data on the medium- to long-term safety of these medications which is concerning.
Natural alternatives to Ozempic and GLP-1 medication
The effectiveness of GLP-1 medications highlights something important. When you target blood sugar, insulin, and appetite regulation, weight loss becomes significantly easier with PCOS.
However, while insulin resistance is a common cause of PCOS, it’s not the only driver. There are at least four known types of PCOS and at FUTURE WOMAN we see an even more complex and personalised picture when working with PCOS clients. Therefore, the best natural approach needs to be personalised to you.
At FUTURE WOMAN, we focus on identifying why your body is holding onto weight, so you can finally lose it in a way that is sustainable and aligned with your hormones.
Read more about the benefits of testing for PCOS.
If testing shows insulin resistance, which is the case for many women, your plan would focus on improving that pathway directly.
This might include:
- Blood sugar support: We’ll tell you exactly how much protein you should be eating, how to structure your meals across the day and share simple habits to reduce glucose spikes.
- Targeted supplementation: Our practitioners will recommend targeted supplements, which might include myo-inositol, berberine or magnesium, which can support insulin sensitivity and metabolic health when taken correctly.
- Lifestyle recommendations: We’ll suggest a unique exercise plan for you, as well as targeted stress reduction practices, as part of your 12 week plan.
- Progesterone therapy: We can prescribe cyclical body identical progesterone therapy in our bHRT clinic, which has been shown to be effective at restoring ovulation, lowering DHT (the active form of testosterone), and even speeding up metabolism. Learn more about how progesterone can help at our FUTURE WOMAN bHRT clinic.
This is how we replicate the effects of GLP-1 medications, by improving insulin sensitivity, stabilising appetite, and creating a metabolic environment where weight loss becomes easier, without relying on medication long term.
We will also address other common causes of PCOS if they show up in testing, such as stress, inflammation and gut dysbiosis.
Ready to understand what’s actually driving your PCOS?
Take our short symptom assessment to find out which test is right for you.
Take the quizHelen’s story: what happens when you address the root cause
Our client Helen was increasingly frustrated with the advice she was receiving from her GP to just ‘lose weight’. She was feeling too tired to go to the gym and was struggling with constant cravings for sweet foods. By addressing her PCOS drivers through our testing – for Helen she needed support with blood sugar, stress and inflammation – we were able to help her finally lose weight.
As she told us: “For years I struggled to understand why I couldn’t lose weight, and was told by my GP that my BMI was the problem. After doing the Advanced Hormone Test, I finally understood what was actually going on in my body. I now have a clear, personalised plan, and for the first time I feel like my body is starting to respond.”
Rather than relying on appetite suppression alone, our approach focuses on identifying and correcting the underlying drivers, so results were not dependent on a single intervention, and therefore longer lasting.
Conclusion
This is why understanding the drivers behind Ozempic PCOS weight loss is key to achieving sustainable results. To summarise:
- GLP-1 medications work because they target real biological pathways, particularly insulin sensitivity, blood sugar regulation, and appetite control.
- They are not a magic solution, but they do highlight what actually needs to be addressed for women with PCOS to lose weight effectively.
- By understanding your own biology and taking a personalised approach, it is possible to support these same pathways naturally and achieve sustainable results.
- If you are ready to understand exactly what is driving your weight, take our Advanced Hormone Test and get a personalised plan designed for your body.




