Discover the key differences and similarities between PCOS and endometriosis, how to know if you have either condition, and how to approach treatment.
Quickly find what you need
PCOS and endometriosis: how do you know if you have them?
Polycystic ovarian syndrome (also known as PCOS) and endometriosis are both conditions linked to women’s hormones that affect millions of women around the world.
It is also possible for women to suffer from both conditions: based on our research at FUTURE WOMAN, we believe that around 1 in 10 women with PCOS also have endometriosis.
Let’s look at what PCOS and endometriosis are in turn, starting with PCOS.
What is PCOS?
PCOS stands for polycystic ovarian syndrome, and it is an endocrine-metabolic disorder that affects up to 20% of women worldwide. It’s the most common hormone condition in women of reproductive age and the most common cause of fertility issues related to a lack of ovulation.
PCOS occurs when levels of androgens (sometimes incorrectly referred to as male hormones!) are high, which prevents ovulation from occurring. This leads to irregular or missing cycles, and other day-to-day symptoms.

Common signs and symptoms of PCOS
The most common signs and symptoms of PCOS are:
- Irregular or missing periods
- Excess body hair growth (hirsutism) or head hair loss
- Acne (especially around chin and jawline)
- Weight gain (around abdomen)
- Bloating
- Sugar cravings
- Fertility issues
- Skin tags
- Skin discoloration or pigmentation
- Mood swings, anxiety or depression
- Fatigue
Importantly, you’ll notice that pain is not a symptom of PCOS.
Check your PCOS symptoms now
What is endometriosis?
Endometriosis affects as many as 1 in 10 women of reproductive age. It is a condition where areas of tissue that are similar to the endometrium (lining) of the uterus grow in places other than the uterus. They can occur anywhere in the body – the bowel, bladder and throughout the pelvis, for example. The most common sites are around the uterus and ovaries and on the fallopian tubes.
Signs and symptoms of endometriosis
The two most common warning signs of endometriosis are pain (commonly pelvic pain) and heavy periods. Other symptoms include:
- Bladder issues – urgency, frequency, pain – similar to a UTI.
- Bowel problems – constipation and/or diarrhoea.
- Bloating – symptoms like bloating and constipation can often be mistaken as IBS.
- Nausea and vomiting – this is commonly associated with the pain of endometriosis.
- Headaches.
- Fatigue.
- Low-grade fever.
- Bleeding between periods.
- Infertility and recurrent miscarriage.
Check your endo symptoms now
Are any symptoms of PCOS and endo the same?

PCOS and endometriosis share some similar symptoms. This means it may be hard to tell what condition you have, or if you have both. These overlapping symptoms include:
- Fatigue
- Bloating
- Heavy periods (can be present with PCOS)
- Bleeding between periods
- Fertility issues
One symptom that is not shared between the two conditions is pain – this is only a symptom of endometriosis.
What causes PCOS and endometriosis? Let’s look at the underlying causes and influences of PCOS and endometriosis next.
What causes PCOS and endometriosis?
The underlying drivers of PCOS
PCOS is a condition involving high levels of androgens (sometimes incorrectly referred to as ‘male hormones’), which suppress ovulation.
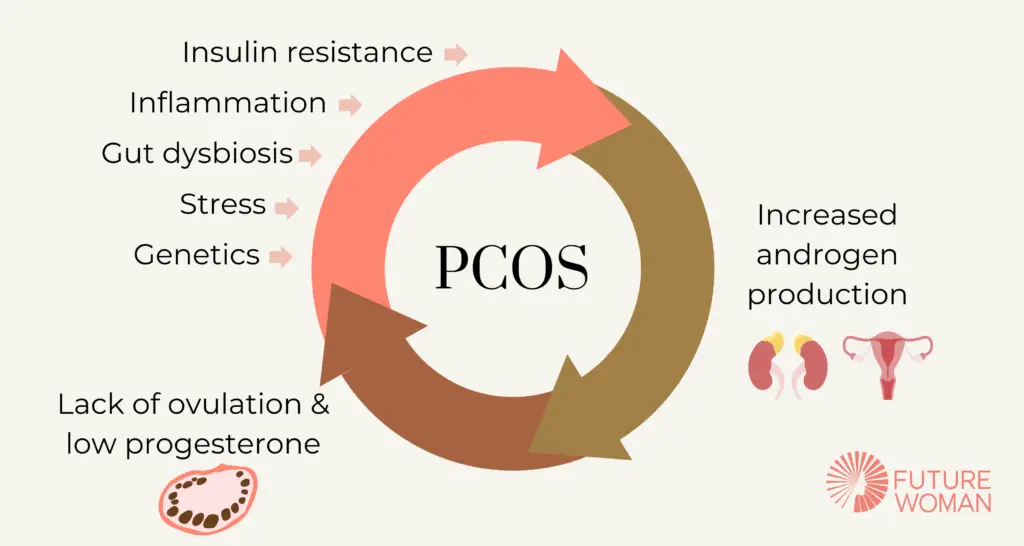
Underlying drivers of PCOS include:
- Insulin resistance: The majority of women with PCOS (50%-90%) are insulin resistant, which can lead to raised androgens. (Read more about insulin resistance and PCOS here)
- Inflammation: PCOS is associated with chronic low-grade inflammation in the body.
- Gut dysbiosis: Higher levels of bacteroides and gram-negative bacteria (LPS toxins) have been seen in women with PCOS and are linked to an increased risk of insulin resistance, inflammation and increased androgens.
- Stress: Stress causes the release of cortisol (a stress hormone) which can increase blood sugar levels, insulin resistance and inflammation, all of which can contribute to an excess of androgens.
- Genetics: More research is needed, but there may be a genetic link involved with PCOS.
The underlying drivers and influences of endometriosis
The causes of endometriosis are complex and still not fully understood. At FUTURE WOMAN, we see the following as common drivers that influence endometriosis
- Inflammation: Endometrial-like tissue, outside its normal location, forms lesions which activate an immune response. In endometriosis, the immune response may be insufficient at removing these lesions. The lesions stimulate inflammatory cells which create inflammation, leading to pain and disruption of normal hormonal regulation.
- Unopposed estrogen: Estrogen is a main driver of the inflammation and pain in endometriosis. This is because estrogen plays a very important role in how endometrial tissue grows, it essentially causes it to thicken which in turn can increase pain, heavy periods and inflammation. Women who have endometriosis typically have high estrogen (in particular estradiol) levels.
- Progesterone resistance: Some women with endometriosis have been shown to be resistant to progesterone. Low progesterone can also cause unopposed estrogen which can worsen endometriosis.
- Stress: Stress can impair the function of the immune system, causing inflammation which worsens all endometriosis symptoms.
- Gut dysbiosis: High levels of gram-negative bacteria (LPS toxins) can disrupt normal immune function, leading to an inflammatory environment which can exacerbate endometriosis. Interestingly, antibiotics have been shown to help treat endometriosis in some women, supporting the theory that gut dysbiosis plays a role.
- Genetics: Finally, it is thought that there is a genetic component to endometriosis and that endometrial tissue outside the uterus may be present before birth.
Can these conditions influence each other?
As seen above, inflammation, gut dysbiosis and stress are drivers of both PCOS and endometriosis. Because of these shared risk factors, as well as changes in sex hormone production, women with endometriosis might have an increased risk of PCOS or vice versa.
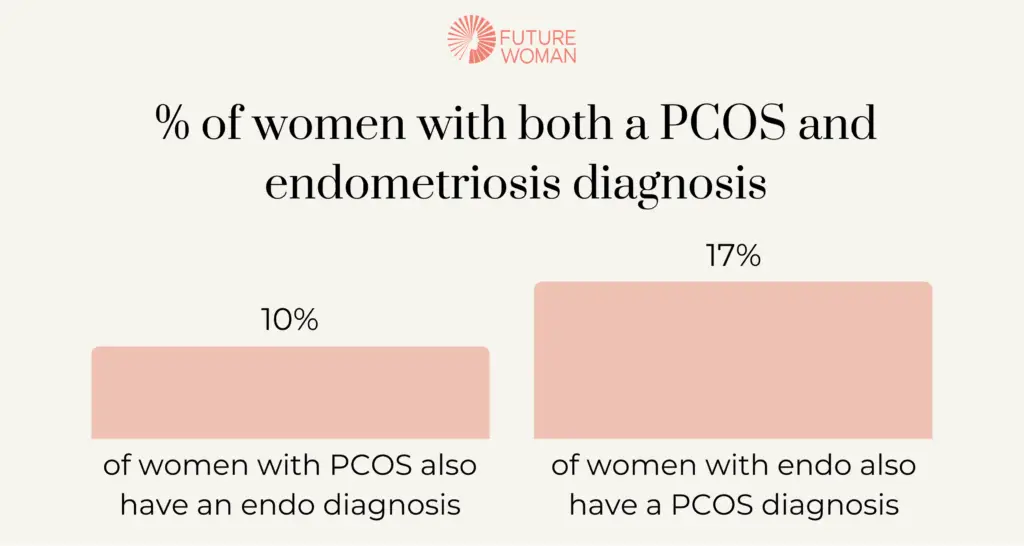
In a survey carried out by FUTURE WOMAN of 4,000 adult women, 332 were previously diagnosed with PCOS and of these 10% were also diagnosed with endometriosis. 192 women were diagnosed with endometriosis and of these 17% were also diagnosed with PCOS. The actual number may be higher as endometriosis is well known to be underdiagnosed.
Can PCOS cause endometriosis? Or vice versa?
There are a few factors that can influence each condition in turn.
- High androgens in PCOS can lead to high estrogen: Androgens are converted to estrogen via an enzyme called aromatase. So high circulating androgen levels, as seen in PCOS, can lead to high estrogen levels which in turn can influence endometriosis. Aromatase has also been shown to be more present in women with endometriosis, and can also lead to problems with the way estrogen is metabolised. It can lead to higher circulating levels of a phase 1 estrogen metabolite called the 16-OH, which has more proliferative effects. Read more about estrogen metabolism.
- Low progesterone in PCOS can increase inflammation: Progesterone is an anti-inflammatory, so lack of progesterone (due to lack of ovulation) in PCOS could make endometriosis, an inflammatory condition, worse.
- Low progesterone in PCOS can result in unopposed estrogen: Even when levels of estrogen are normal, if they are not balanced out by progesterone, the effects of estrogen can be more potent which can worsen endometriosis symptoms.

Fertility and PCOS and endometriosis: is it harder to get pregnant?
Let’s look at how PCOS and endometriosis might affect fertility.
Does PCOS affect fertility?
About 70% of women who have PCOS have difficulty conceiving mainly because they do not ovulate, or ovulate very infrequently. They also may not produce progesterone to support pregnancy in its early stages.
Does endometriosis affect fertility?
30-50% of women with endometriosis may experience infertility because it can alter the immune system, change the hormonal environment around the eggs and inhibit implantation of an embryo.
There are many things that can be done to manage PCOS and endometriosis to help with fertility and day-to-day symptoms. Let’s look at how we address each of these conditions at FUTURE WOMAN.
How do you address PCOS and endometriosis?
If you believe you may be suffering with PCOS, endometriosis or both, it’s important to address the root cause for lasting change. As such, our recommended next step is to investigate and address the root causes of your condition or conditions using comprehensive hormone testing.
PCOS and hormone testing
With PCOS, hormone testing is important for two reasons. The first is that it’s only by testing androgen levels that you can confirm you really have PCOS – an ultrasound is not enough to diagnose PCOS. Secondly, it’s important to test for possible underlying drivers of your PCOS so that you can treat it at a root cause level.
We recommend a comprehensive hormone test like the Advanced Hormone Test, which tests for androgens, estrogen, progesterone as well as common underlying drivers of PCOS such as stress hormones, nutrients, gut dysbiosis and inflammation. It comes with a personalised plan with supplement, diet and lifestyle recommendations to address your symptoms, prepared by an expert nutritionist.
Endometriosis and hormone testing
Comprehensive hormone testing is also vitally important for endometriosis. We recommend testing with a hormone test such as the Advanced Hormone Test, which assesses not only estrogen, progesterone and other reproductive hormones, but also markers for inflammation, stress and gut dysbiosis which as we’ve seen can play a role in driving endometriosis.

Should you address PCOS or endometriosis first?
If, as a result of testing, we believe you are struggling with both PCOS and endometriosis, we will likely address endometriosis first, before PCOS.
This is for two key reasons. The first is that the symptoms of endometriosis are typically more debilitating when it comes to day-to-day life. The second is that treating PCOS can, in some cases, drive estrogen levels higher, which could make your endometriosis worse.
As we have seen, some of the underlying drivers of PCOS and endometriosis are the same, such as inflammation and stress. We would typically look to address inflammation as a priority, since it plays such a key role in both conditions. Targeting stress can also be beneficial for both diseases to balance cortisol production.
What about the pill for PCOS and endometriosis?
If you go to your GP, you’ll likely be recommended the contraceptive pill to help with symptoms of PCOS, endometriosis, or both. However, while the contraceptive pill can help with the day-to-day symptoms of both PCOS and endometriosis, it does not address the root cause and therefore symptoms will return (and sometimes worse) when you stop taking it.
For women with endometriosis, the contraceptive pill is ineffective in 33% of cases because they are progesterone resistant (and the hormones in the pill are progestins)
For women with PCOS, in our experience often the pill can make symptoms worse. This is because many of the synthetic progestins in the pill are derived from androgens (which are already high in PCOS).
Finally, many women are diagnosed with PCOS or endometriosis when they are having problems with fertility, so the pill is not an option for them.
Can I still test my hormones if I am on the contraceptive pill?
Yes, you can still test your hormones with the Advanced Hormone Test if you’re on the pill! Although we won’t be able to look at your estrogen and progesterone levels as these are suppressed by the pill, there are many other analytes we can test. Markers for androgens, gut dysbiosis, nutritional deficiencies, hormone metabolism, inflammation and cortisol can all be looked at to assess your overall health picture.
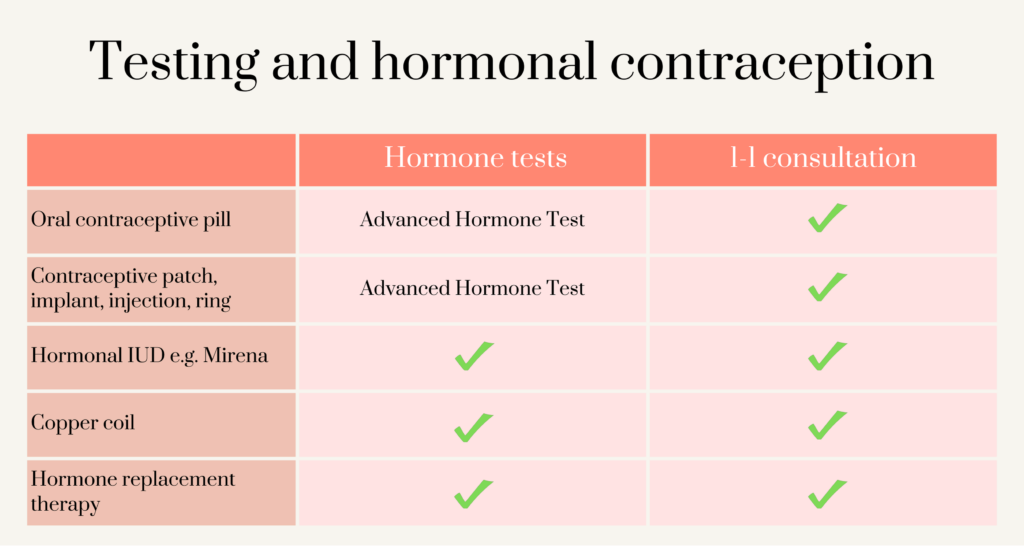

What if I want to come off the contraceptive pill?
If you have decided you want to come off the pill we recommend waiting 3 months before testing, to allow your hormones to get back to their baseline levels.
In the meantime, we would recommend a consultation with one of our nutritional therapists so that we can support you with the transition and help you to manage symptoms.
Next steps
- Confirm if you really have PCOS by testing. We see many women who have been misdiagnosed with PCOS based on ultrasound alone. You need irregular or non-ovulatory cycles AND raised androgens to have PCOS.
- Choose a comprehensive hormone test to identify and address the root drivers. As we’ve covered in this article, there are many possible drivers of PCOS and endometriosis. Testing with a thorough hormone test like the Advanced Hormone Test can help you understand your unique hormone picture and we can then address those drivers in your free personalised plan.
- If you’re on the pill you can still test your androgens, stress hormones and other markers to address the root cause of your PCOS or endometriosis, or chat to an expert in a 1-1 consultation.
References
Baker, J. M., Al-Nakkash, L., & Herbst-Kralovetz, M. M. (2017). Estrogen-gut microbiome axis: Physiological and clinical implications. Maturitas, 103, 45–53.
Jiang, I., Yong, P. J., Allaire, C. & Bedaiwy, M. A. (2021). Intricate Connections between the Microbiota and Endometriosis. International journal of molecular sciences, 22(11), 5644.
Mori, T., Ito, F., Koshiba, A., Kataoka, H., Takaoka, O., Okimura, H., Khan, K. N., & Kitawaki, J. (2019). Local estrogen formation and its regulation in endometriosis. Reproductive medicine and biology, 18(4), 305–311.
Reis, F. M., Coutinho, L. M., Vannuccini, S., Luisi, S., & Petraglia, F. (2020). Is Stress a Cause or a Consequence of Endometriosis?. Reproductive sciences (Thousand Oaks, Calif.), 27(1), 39–45. https://doi.org/10.1007/s43032-019-00053-0
Sadeghi M. R. (2022). Polycystic Ovarian Syndrome and Endometriosis as Two Evil Extremes of Health Continuum. Journal of reproduction & infertility, 23(1), 1–2.
Schliep, K. C., Ghabayen, L., Shaaban, M., Hughes, F. R., Pollack, A. Z., Stanford, J. B., Brady, K. A., Kiser, A., & Peterson, C. M. (2023). Examining the co-occurrence of endometriosis and polycystic ovarian syndrome. AJOG global reports, 3(3), 100259.
Xue-ya QIAN, Hao WU, Xiao-wei XI (2011) Is There A Relationship between Polycystic Ovary Syndrome and Endometriosis? Journal of Reproduction and Contraception, 22(3),
Zizolfi, B., Foreste, V., Gallo, A., Martone, S., Giampaolino, P., & Di Spiezio Sardo, A. (2023). Endometriosis and dysbiosis: State of art. Frontiers in endocrinology, 14, 1140774.







